We do more than just manage your receivables. Our advanced AR service integrates seamlessly
into your
existing workflow, while we proactively tackle denials and underpayments, employing
rigorous accounts
receivable follow-up measures with payers.
KG Invicta Consistently Delivers, Guaranteed!
Average denial rate
Reduced below
5%Days in
Accounts Receivables
Increase in
Collection rate
95%How We Enhance Your AR Management
Precision Tracking: Monitoring claims, especially those that cross the 30-day threshold, for timely action.
Engaging with Payers: Consistent interactions with payers to resolve underpaid claims to ensure every dollar is accounted for.
Prompt Error Addressing: Rapid identification and rectification of discrepancies in rejected claims.
Upholding Data Integrity: Through meticulous cross-verification of data sources and medical code validations.
Patient Relations: Maintaining active communication channels with patients regarding their outstanding balances.
Enhanced Efficiency: Accelerating AR cycle times and reducing the aging of outstanding claims.
Decoding Our AR Management Process
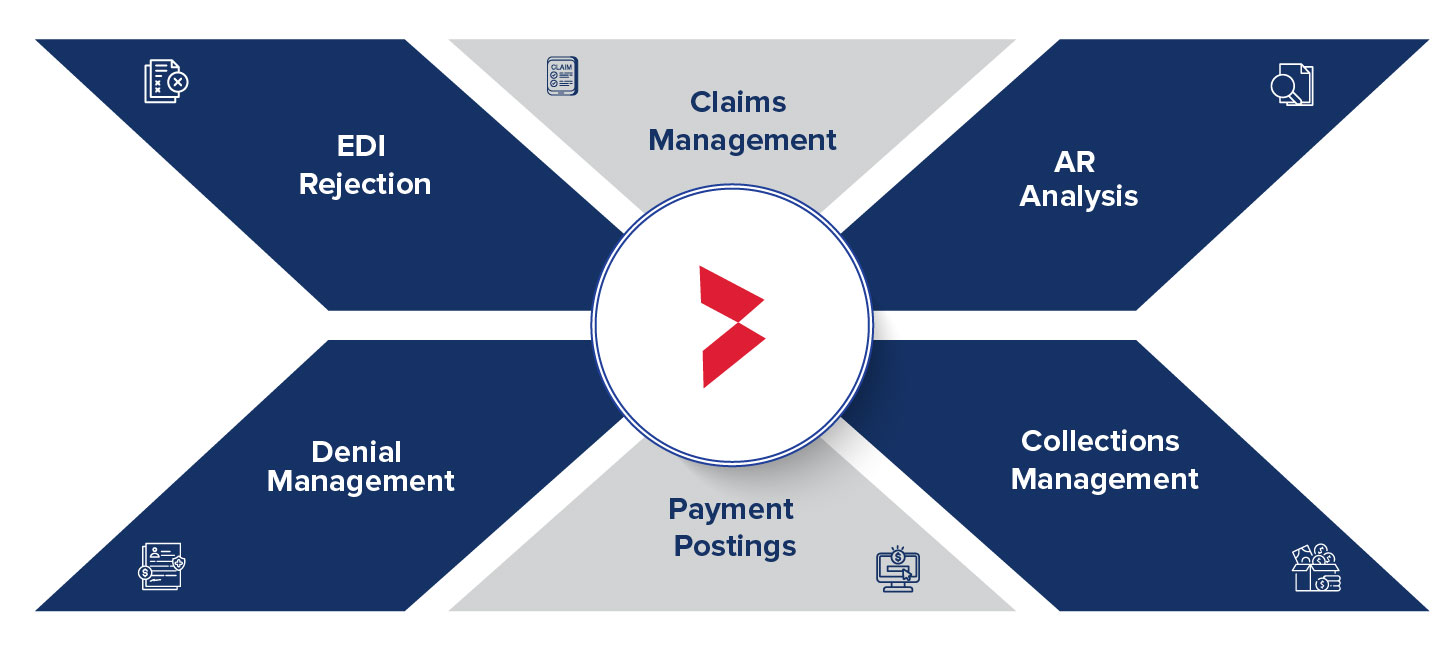
Stay at the forefront of the healthcare sector with financial processes that are as streamlined and efficient as your medical services.
We help you uncover the full potential of your operational efficiency.
Reach out to us for better ideas and stragies for an effective RCM.
Schedule a conversation with our expert.










